What You Need to Know About Perimenopause & Birth Control
Birth control is something many women take to prevent pregnancy and help with other conditions. However, as you enter perimenopause, you might have some questions about birth control. Our providers are here to answer your questions and help you make decisions about your health before, during, and after perimenopause. It’s important to discuss the particulars of your situation with one of our medical providers. However, we do have a general guide to help answer some common questions about birth control and perimenopause.
Summary
- Perimenopause is the transition period before menopause when hormone levels begin to fluctuate. It typically starts in women in their 40s but can begin earlier and last several years. Menopause is officially diagnosed after 12 consecutive months without a menstrual period.
- Yes, pregnancy is still possible during perimenopause because ovulation can continue even when periods become irregular. Because of this, many healthcare providers recommend continuing contraception until menopause is confirmed. This usually means waiting until a full year has passed without a period.
- Hormonal birth control can sometimes mask the symptoms of perimenopause. Birth control that contains estrogen and progesterone regulate hormone levels and may produce withdrawal bleeding that looks like a normal menstrual cycle. This can make it harder to know when natural menopause has occurred. As a result, some women may not realize they have entered menopause while still using birth control.
- In some cases, hormonal birth control may help reduce perimenopause symptoms. Some providers will prescribe birth control to regulate cycles and improve some symptoms in the transition to menopause. But the best option depends on a multitude of factors.
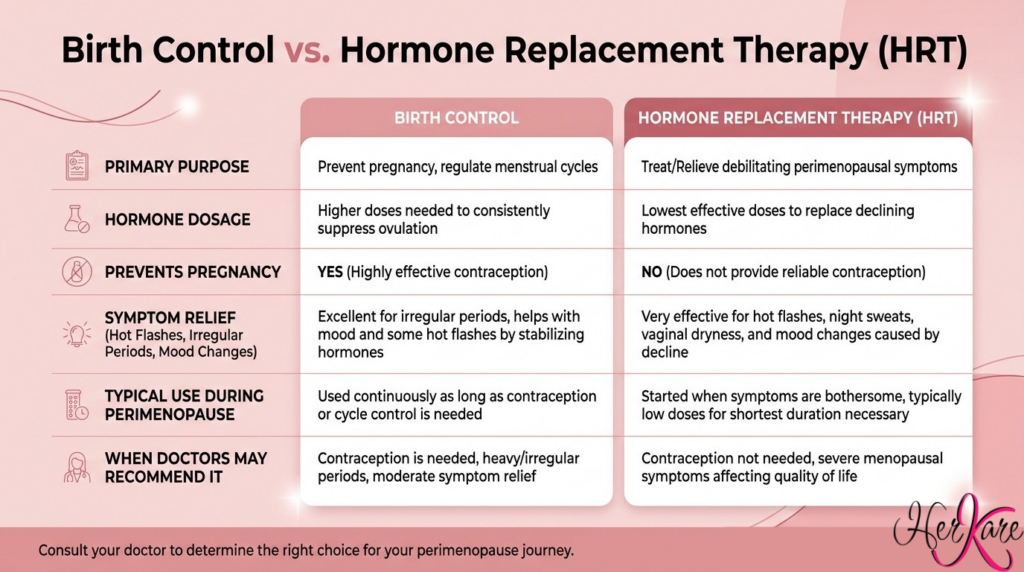
- Birth control is designed to prevent pregnancy and typically contain higher amounts of hormone levels to suppress ovulation. Menopause hormone therapy is intended to relieve symptoms such as hot flashes and unrestful sleep. Hormone replacement therapy usually contains lower hormone doses than birth control. At HerKare, a provider can help you determine which option is best for you during perimenopause.

You may still need birth control during perimenopause to prevent pregnancy.
What is Perimenopause?
First, let’s clarify what we mean by “perimenopause.” The terms perimenopause and menopause are often used synonymously, but they are actually different stages of your life. Perimenopause is the time leading up to menopause. Menopause is when you have gone 12 consecutive months without a period.
During perimenopause, your hormones may start to fluctuate more, but you’re still producing a fair amount of both estrogen and progesterone. When you reach menopause and postmenopause, your ovaries produce very little of these hormones and stop releasing eggs. Perimenopause typically begins in your 40s. It usually lasts around four years before you reach menopause. However, this can be longer or shorter for different women, even up to 10 years or more. The average age for menopause is 51 years old, though it can come earlier or later.
Symptoms of Perimenopause
There are many symptoms that can point to perimenopause. While there is no one test or sign that you’ve started perimenopause, some symptoms can signal that you may be in perimenopause.
Some symptoms of perimenopause include:
- Irregular periods
- Fatigue
- Spotting or breakthrough bleeding
- Breast tenderness
- Headaches
- Low libido
- Difficulty concentrating (“brain fog”)
- Hot flashes
- Night sweats
- Vaginal dryness
- Mood changes
If you’re dealing with these symptoms, then it may mean that you’re starting the transition to menopause. You can talk to one of our treatment providers about your symptoms to determine whether you might be in perimenopause and how we may be able to help reduce or relieve your symptoms.
Can You Still Get Pregnant During Perimenopause?
Now, it’s a common misconception that you can’t get pregnant during perimenopause. This is incorrect. You can absolutely still get pregnant during perimenopause. Your body typically still ovulates during perimenopause. While periods might be irregular or different during perimenopause, pregnancy is still a risk with unprotected sex. Therefore, many women still need contraception in the years leading up to menopause if they don’t wish to become pregnant. The risk of becoming pregnant generally doesn’t go away until after you’ve reached menopause, one year after your last period. Hormonal birth control is one of the most common forms of contraception, so many women continue to take these medications up until they reach menopause.
Birth Control May Mask Symptoms of Perimenopause
It’s important to note that hormonal birth control, like the pill, can actually mask symptoms of perimenopause and menopause. Hormonal birth control uses synthetic versions of female hormones estrogen and progesterone, which control menstruation, pregnancy, and more. Hormonal birth control can help regulate hormone levels to control periods and reduce the risk of pregnancy.
Symptoms of perimenopause and menopause are typically caused by fluctuating and declining levels of estrogen and progesterone in your body. Therefore, if you’re taking hormonal birth control, it may mask some of the symptoms of perimenopause by replacing your natural hormones with synthetic versions. Your symptoms may not be as noticeable if you’re still on hormonal birth control when you start perimenopause.
Also, many women who do experience symptoms may not associate them with perimenopause, as birth control side effects can be very similar to perimenopause. For instance, changes in mood and sex drive can be side effects of birth control and symptoms of perimenopause.
Even after menopause where your ovaries stop producing estrogen and progesterone, birth control can make it appear that you are getting regular periods. When taking combination birth control with both estrogen and progesterone, you may experience withdrawal bleeding that mimics your period, even though you’ve reached menopause.
Hormonal Birth Control May Help Reduce Symptoms during Perimenopause
In a similar vein, some women notice that their perimenopause symptoms get better after beginning hormonal birth control. Some doctors may even prescribe birth control during perimenopause to help with symptoms even if you’re not looking for a contraceptive. Of course, this depends on your individual circumstances. Some women may not benefit from birth control during menopause, and for some the risks outweigh the benefits. However, the hormones in birth control may help some women feel better during perimenopause.
As you transition into menopause, your hormone levels may fluctuate quite a bit. This can cause many symptoms that affect your quality of life, such as hot flashes and mood changes. Birth control can help regulate your hormones to reduce these fluctuations. This may, in turn, help alleviate some of your perimenopause symptoms.
How to Know if You’ve Transitioned to Menopause while On Birth Control?
So, if you take birth control during perimenopause and it can mask symptoms and even cause bleeding that mimics a normal menstrual period, how do you know if you’ve reached menopause? In most cases, stopping birth control can help you determine if you have reached menopause. Just keep in mind that until you are sure you have gone for one year without a period, you may need other forms of contraception, such as condoms, to help prevent pregnancy. Even if you have gone several months without a period, you may still be perimenopausal and still able to get pregnant. Talk to one of our treatment providers about your specific circumstances.
When Should Perimenopausal Women Stop Taking Birth Control?
You might be wondering if there is a certain time you should stop taking birth control after you enter perimenopause. Once again, this is personal, so it’s important to discuss the specifics with one of our treatment providers.
However, many doctors do recommend some women stop birth control at the average age of menopause (51 years old) to determine if they’ve reached menopause yet. Also, it’s important to understand that with age, the risks of birth control can get higher. For instance, some hormonal birth controls can increase your risk for blood clots, stroke, breast cancer, heart attacks, and other health conditions. Therefore, our treatment providers may recommend stopping or switching hormonal birth controls based on your risks, even if you’re not in perimenopause.
What’s the Difference Between Hormone Therapy and Birth Control?
You may have heard of women taking hormone therapy during and after perimenopause. If birth control typically contains hormones, what is the difference between birth control and hormone therapy for menopause?
Hormone therapy and birth control have different purposes and do different things in your body. Therefore, one might be better than the other for your circumstances.
Generally speaking, birth control is primarily to prevent pregnancy (though you might also use it for other things like regulating your cycle, reducing PMS symptoms, or even to help with hormonal acne). Hormonal birth control typically contains synthetic forms of estrogen and progesterone that are much stronger than you would find in the average hormone therapy medication. Also, most forms of hormonal birth control override ovarian function, meaning they tell your ovaries to take a break while they provide the hormones instead.
By contrast, hormone therapy is primarily used to help reduce symptoms of menopause. These medications help supplement what your ovaries naturally produce. HRT also typically provides much less estrogen and/or progesterone than birth control medications, providing the minimum amount needed to help with your symptoms. Hormone therapy also isn’t an effective form of contraception.
Does Birth Control Delay Menopause?
Another question you have is whether taking hormonal birth control delays menopause. After all, if you might have fewer symptoms and might continue bleeding each month while taking the pill, that certainly sounds like you’re not in menopause. However, this is another common misconception.
Birth control doesn’t stop, delay, or turn back the clock on menopause. Menopause is the end of your reproductive years, meaning your ovaries stop releasing eggs and producing as much estrogen and progesterone. As far as we know, there is nothing we can do or take to prevent menopause from happening. So, while birth control might mask the signs and symptoms, it won’t make your ovaries continue to function as they did in premenopausal years.
Comprehensive Women’s Health Care from Our Providers at HerKare
Our treatment providers at HerKare are here to help you address your health and feel your best. We can help you make important decisions around birth control, health risks, and symptom relief during and after menopause. Our team is dedicated to providing high quality women’s health care at every stage of life. Make an appointment today to learn more and discuss your health with one of our medical providers.
